5 Surprising Myths and Options for your Utah Hospital Birth
So. You’re planning to birth at the hospital (or maybe feeling nervous about *maybe* needing to transfer to one if you’re planning to birth at home or at one of our fantastic birth centers). If you’re like me (or many of my client family), you might believe that birthing in one of our Utah hospitals means you’re really, really limited in your birth options. And you CRAVE those options, and the feeling of empowerment you get when you make your own decisions. But with the way everyone talks… well, it doesn’t feel like there are options there.
Well, take a deep breath, friend – remember, I’m here for you! Truth is, you DO have options in a hospital birth, and I believe (FIRMLY) that it’s your birth wherever you go. SO, let’s dispel these myths, and re-ground yourself in 5 of the many options you have in a hospital birth – because every parent deserves to go into their birth feeling in charge of their body, choices, and birth experience. (Remember – your provider is there for YOU, so if these spark questions for you, totally bring them to your next prenatal!)
Utah Hospital Birth Options and Myths
Myth #1: If you go the hospital, you’ll have to birth in the bed.
I’ll be honest: this myth exists for a reason. For many providers, this is the only way they’ve ever caught babies, and the only way they’ve been trained to catch babies. *Cue the wide-eye emoji.* Frankly, it’s what’s most convenient for them, and has the least liability. (I think they’ve made the bed one of the softest spots in an L&D room for a reason). On top of that, many hospital providers primarily support birthers that get epidurals (and if you choose to have an epidural, that does mean also choosing to birth in/on the bed for safety reasons). So hospital bed-birth is what hospital staff is used to!
But. Just because that’s what’s commonly done or what your provider is used to doesn’t mean that you have to birth in the bed (and hopefully, if you don’t want to birth here, your provider is plenty confident in catching babies wherever they come). Which leads us to…
Option #1: You can birth wherever you choose in your hospital room.
And your provider should support that. So long as you don’t have an epidural blocking sensation to your legs, you can go wherever you want in your birth room! That could be in the bathroom right on the toilet, on the floor, in the shower, in the bathroom doorway, on the couch they set up for your partner to sleep on, next to the bed (like Emma’s birth), or on the bed itself (it is still a soft-ish, flexible, great place to birth).
If you do have an epidural, well, that leads us to our next myth!
Myth #2: If you get an epidural (or not), you’ll can only push on your back (aka in lithotomy position).
While you can totally choose to push that baby out on your back (and given the choice, some 100% feel most productive or comfortable there), that’s not the only option you have in a hospital birth. Even with an epidural, there are LOTS of options to both push and labor in (aka option #2).
Option #2: There are so, so many positions to push out a baby in!
My generic starter list for you:
- On your side
- Sitting on the bed
- Supported squat (by your partner, a birth stool, your doula, or an awesome L&D nurse)
- Standing up (like Emma’s birth)*
- On your hands and knees
- With one foot up on the bathtub/couch/stool/squat bar
With an epidural, you’ll just need more support to get and stay in different positions. (*Standing is the only position I see as unsafe with an epidural, even with support.) Changing positions can be especially helpful when pushing for an extended amount of time (even some subtle adjustments can make a big difference).
Birth Plan Question: where and how do you imagine being most comfortable birthing? Is your provider comfortable supporting you there?
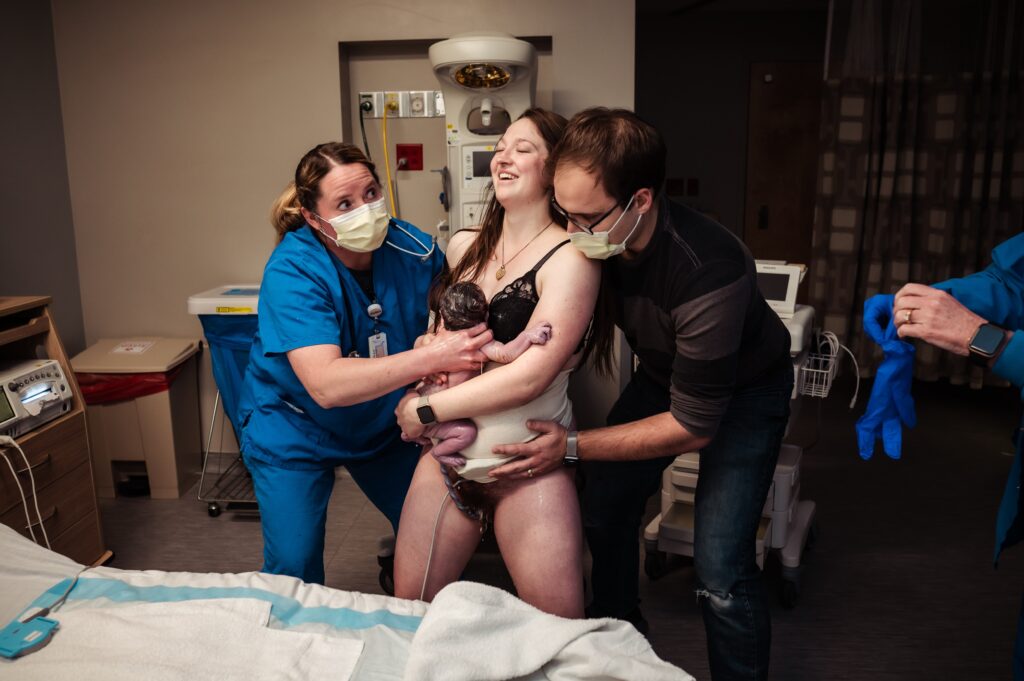
Myth #3: An epidural is the only form of pain relief available at the hospital.
While it may be the first form of pain relief offered to you at the hospital, an epidural is not the only form of pain relief available to you!
Option #3: You can find relief from the intensity of birth in LOTS of different ways.
If your room has a shower or a tub, you’ve got hydro-therapy! If you’ve got a partner, doula, or friend there, you’ve got massage therapy, emotional support, and acupressure. You can bring a TENS unit, your favorite scents (aromatherapy), and/or your favorite music. Even simply moving around and into various positions can provide pain relief; some positions will likely feel less intense than others. Many hospitals also offer nitrous oxide and narcotics (early enough in labor) as well as spinal blocks (I’ve primarily seen this with cesarean birthers).
Also remember that the intensity of birth is usually mental as well as physical – mindfulness, hypnobirthing, emotional support, and other mental coping strategies can also be incredibly valuable. (Mindful Birthing is a new favorite mental birth prep book of mine – and all the mindfulness practices apply for life and parenthood, too!)
Birth Plan Question: how do you cope with discomfort, pain, anxiety or fears? How can you bring some of those coping skills into your birth space?

Myth #4: OB’s are for hospital birth, you can only have a midwife if you’re having a home/birth center birth.
This is also *partially* true; here in Utah, you’ll only find OB’s (obstetricians) supporting hospital births, and midwives are the only kind of provider that supports out-of-hospital birth. However, midwives (CNM’s, specifically) also support hospital births!
Option #4: You can choose either a midwife or OB as your provider for a hospital birth.
Typically, midwives are going to be more comfortable with physiological birth than their OB counterparts and use the shared model of decision-making (aka you make decisions about your birth together vs your provider telling you what to do). They love supporting both unmedicated and epidural birthers, and are the experts in low-risk birth. My hospital midwife for Emma’s birth also worked often with the OB counterparts at her practice – so I knew if my birth ever became high risk, or if we ever chose a cesarean, she would have trusted friends to come help her support us (vs a stranger) and be able to keep advocating and caring for us.
OB’s are the experts in managing more complex, high-risk birth, and the only providers trained in performing cesarean birth. Though there are some OB’s out there that are familiar with supporting unmedicated births, most are only familiar with managing medicalized birth (though the uncomfortable-with-unmedicated-birth OB’s can sometimes be the absolute best at supporting family-centered cesareans!).
My OB for Eleanor’s birth was much more the latter – nice, but wholly unhelpful and likely the driving force behind the nurses pushing to check my cervix every 2-3 hours (numbers were what she was used to working with, not other emotional measures of how birth is progressing). The OB I consulted with in Emma’s pregnancy (for my Factor V Leiden gene) felt like much more the former – he presented all the options, owned to his bias, and thoroughly seemed to want to support me as a person, even in his rush of meeting with a LOT of people that day.
Myth #5: sure there are options for vaginal birth, but I’m having a cesarean, and my provider has to make all the decisions about that!
Or, from a different perspective: I can feel good birthing in the hospital, can make decisions, have options, etc.. UNLESS I end up in a c-section. Then it’ll be traumatic, I’ll have failed in all my goals, and I’ll have to hand over decision-making to someone else.
Let’s get real clear here: cesarean births are not inherently traumatic or negative, and never have I ever heard of a c-section where the birthing person FAILED in having one. However, c-sections can certainly be traumatic and negative experiences, especially when the birthing family feels that they had no choice in the matter, or felt unsupported, invalidated, or bullied.
I’ve also noticed that some cesarean birth families aren’t given the same celebration or support as if they’d given birth vaginally – whether from someone who might believe that a c-section is the easy way out or from the hospital staff that happily welcomes doulas and birth photographers into the hospital birth space… but not into the OR (cause cesarean birth isn’t worth honoring with professional documentation, right? And you definitely don’t need emotional support *eye roll*).
What can help make the difference between trauma and positive, from routine surgery to beautiful, life-changing birth experience is that feeling of CHOICE, trust, and support. (And, ya know, having a provider you absolutely love and trust.)
Option #5: you can still claim decision-making power in a cesarean birth!
After all, cesarean birth is still birth! And you still deserve decision-making power about your body. That can look like simply choosing to trust your provider’s choices on everything and going with the flow, but it can also look like:
- doing something meaningful as you prepare for your cesarean (playing music, having your favorite scents, extra support people, documentation, reading a book or writing a letter to your baby – the possibilities are endless here!)
- choosing to play music in the OR
- deciding what day you (at least originally) schedule your cesarean
- choosing who comes to support you in your birth space: partner, doula, photographer, etc
- what kind of communication you want from the medical staff (do you want a play-by-play of what’s happening? Or more quiet?)
- having a clear drape to see baby right after they’re born
- assisting in pulling baby out (maternal-assisted cesarean; it’s tricky in terms of maintaining the sterile field, but possible!)
- Partner announcing baby’s sex or name
- Skin-to-skin and breastfeeding in the OR
- Partner and baby staying with you as you’re stitched up (or sending them back to your room to have some space)
- Keeping your placenta for a placenta tour, print, or other meaningful tradition
- Doing something meaningful in the recovery room (a special post-op snack, music, special scents or blankets, documentation, support people, breastfeeding, singing a song to baby – again, the possibilities are endless here)
And this isn’t even close to an exhaustive list! Your provider and doula should be able to help you brainstorm and think through what things could be meaningful for you in helping the experience (planned or not) feel supported and more positive.
Side note: having options is certainly easier when things aren’t emergent (aka it’s not a time-sensitive emergency). But, this is where having backup birth plans really shines; if you’ve thought these things through and shared them with your birth team, then they can help advocate for the most important things when you can’t – so YOUR choices and your voice still are heard.
Birth plan question: if you had/are planning a cesarean, what would help it feel special, supported, and safe? What anxieties do you have about a c-section? What would help you navigate those?
Tada! Let’s recap:
5 Hospital birth MYTHS:
- You have to birth in the bed.
- You have to push on your back
- An epidural is the only pain-relief available
- OB’s are the only hospital providers available
- A cesarean birth doesn’t give space for options.
Instead, remember that there is space for YOUR opinions and choice in all 5 of these spaces (and more, for that matter):
- Where you birth your babe
- How/in what position you birth your babe
- How you find comfort/relief from the intensity/pain of labor
- Who your provider is (and their comfort level with what kind of birth you want)
- And in a cesarean birth (planned or unplanned)
As your doula and photographer, my job is to help you think through all these options before you birth, and to remind you (and the hospital staff) of those options as you birth. (That goes for any and all births – unmedicated, epidural, induced, spontaneous, cesarean – doula support can be valuable for ALL of those.)
Remember that you DO have power to make decisions about your body and birth – in other words, you have birth options at any Utah hospital you might walk into. And remember that you deserve support in those choices. I trust you to make the best decision with the resources available to you. You got this, friend.


